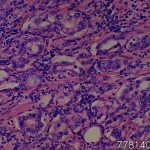
| Product name | Prostate adenocarcinoma |
| Cat. No. | 7781403B |
| No. of samples | 1 |
| Description | Prostate, adenocarcinoma Age/Sex : 73/M |
| Price | 197 EUR |
| 260 USD | |
| 170 GBP |
Product Related Literature
Gleason grading system was to evaluate the prognosis of men with prostate cancer. Incorporated strategies prostate cancer stage helps to predict the other parameters, the estimated values together, to guide the treatment. A more aggressive has given for prostate cancer based on microscopic appearance.Cancers with Gleason score higher Gleason score, it is a poor prognosis. Prostate biopsy is a procedure that is removed from the prostate of male small needle core sample is examined under a microscope for the presence of cancer. Result of blood test, the PSA level is related to the possible presence of prostate cancer rises to, this is usually performed. This can be (DRE) is caused by digital rectal examination abnormal. The PSA and there is room for discussion, PSA screening can be improved by (BPH, benign prostatic hyperplasia), by infection, or to manipulate the prostate catheter surgery or hypertrophy benign. Procedure is usually performed in outpatient, you need a local anesthetic, but some people do report discomfort of biopsy. The most common side effects in the procedure is blood in feces and urine through the blood and a few days in a few weeks and then option ejaculation. Usually a self-limiting, these side effects do not require additional processing.
Procedure can be through the urethra, or through the perineum, do transrectally. And historically transrectally, the most common approach, is being carried out in guidelines tactile finger this. Currently, the most common method of prostate biopsy is the transrectal ultrasound prostate (TRUS) biopsy. Raw extension scheme take 12-14 core through a small needle in a systematic manner from different regions of the prostate from prostate. Antibiotics typically are defined in minmize so the risk of infection. Enema, you may be prescribed to themorning for the procedure. The procedures of the rectum, the doctor inserts ultrasound, to help the biopsy needle into the rectum. The local anesthetic, are then applied to the dental treatment, the prostate, was administered to the surrounding tissue in the same manner as local anesthetic. Spring prostate tissue biopsy needle is inserted into the prostate. Makes a specific sound, local anesthetic if it is satisfied, is held to a minimum discomfort.
In a multicenter study large patient 2299 people, 12 scheme biopsy site, and 44.4% detection rate general, inspection of the cancer detection rate, otherwise using another method for biopsy I am beyond the circuit of all. Ranging from <68% of the hospital in 2 PSA> 20 から 19% in the PSA direct patient, PSA level is related to the detection frequency of cancer. However, biopsy negative, does not guarantee that there is no disease. So you can see an ultrasonic often, prostate cancer, is “blind” systematic TRUS biopsy. This problem is exacerbated in larger prostate patient. Core 14 on-site inspection, additional, are made often “missed” at the site of the common regional front and tip of cancer. The biopsy of the first, is likely to miss the 20-30% of cancer clinically significant. Therefore, the subsequent biopsy is often followed by a negative biopsy of men with a level that sustained elevation of PSA. I have a biopsy detection rate of each session that cancer is reduced. Recently, in order to address this problem, researchers have examined the ability of mitochondrial DNA to help diagnose prostate cancer in biopsy negative.
Since the mid-1980s, for prostate cancer could not be seen on ultrasound due to poor soft tissue resolution, TRUS biopsy is used to diagnose prostate cancer in substantially the blind method. However, it is used for characterizing prostate cancer and identifying good in the middle of 2000 multi-parameter MRI. The study in surgical pathology specimens and correlated MRI, 59% together, showed a sensitivity specificity of 84%, T2, dynamic contrast, the diffusion-weighted images for the detection of cancer. Prostate many tumors missed by biopsy detection of conventional target an MRI guided biopsy. Prostate biopsy “goal” or MRI round, is as follows: two ways. MRI biopsy tract “core” (1) Direct combination of stored real-time MRI, using the biopsy device, fusion ultrasonography (2) (MRI-US). Recognition MRI-US or synthetic vision is disclosed.
When used alone, MRI is performed by the interventional radiologist prostate biopsy guide. Correlation is improved between ascompared MRI guided biopsy to TRUS during the final pathology and biopsy. The fusion NMR U.S. prostate biopsy, prostate MRI raw is executed before, when the biopsy, later, to guide the purpose suspicious urologist, MRI images are merged with ultrasound imaging. U.S. biopsy can be achieved in an office environment with various devices and fusion MRI. It appears better than the standard TRUS biopsy to detect prostate cancer by MRI guided biopsy of the prostate. It than blind systematic biopsy possibility of detecting the cancer is several times have been shown to target biopsy several groups in Europe and the United States was obtained using the fusion image. Potential target cancer is high, and more suspicious MRI, a biopsy.
What is needed from the reader for a fair amount of experience to study prostate MRI. We will continue to evolve as experience MRI scoring system for setting the level of suspicion of cancer have been described, a new modality will increase definitely. By 2013, guidelines for biopsy targeted a program of active surveillance that allows you to use a confirmatory biopsy in that not only concern of increased PSA, you want to add TRUS biopsy traditional staging and more accurate confidence in in spite of the patient registration, patient contains mainly of whom were negative for. In response to the initial biopsy, men towards the biopsy more and more, therefore, the use of pre-biopsy MRI is growing rapidly. The study NIH, the funding has been required, it is in progress to clarify the benefits of prostate biopsy targeted further.